This final post of the 3-part series on boundaries will provide you with definitions for different types of boundaries. It is important to know these differences; doing so allows you to self-appraise how you maintain your sense of self with others. Research mostly focuses on three general types of boundaries: rigid, diffuse, and flexible.
Let’s imagine boundaries as a wall you build up to protect yourself. They can be defined by the following:
Rigid – Walls are very high up, thick, and do not come down
Diffuse – Walls are very low, foggy, and confusing
Flexible: Walls are clear, go down and go up (to different levels) as needed.
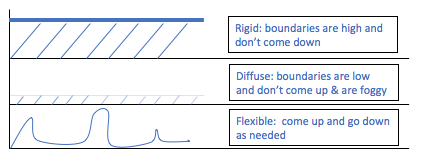
Rigid Boundaries: We might feel protected (especially if we have been through any type of trauma) when we set a rigid boundary without sharing more intimately about our feelings and needs. However, we are closed off to the other when we set a fixed limit — meaning that it’s difficult or nearly impossible for us to connect to others and to have others get close to us (emotionally, physically, etc.). This type of boundary makes it hard for others to understand our feelings and needs as little of ourselves is shared. We also may not be flexible enough to respond to the demands of others.
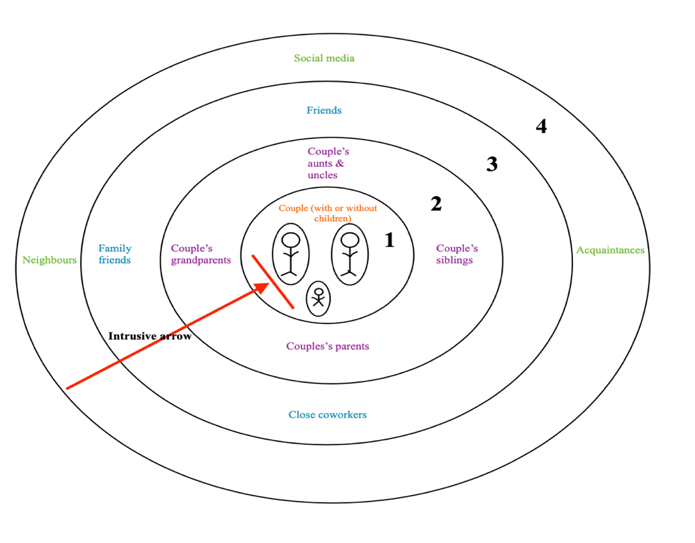
Diffuse Boundaries: When we have diffuse boundaries, we might have difficulties communicating and/or understanding our boundaries (maybe from how you were raised, difficult experiences with limits). With diffuse boundaries, our borders are foggy, unclear, and are not defined. This particular boundary is difficult in relationships because you most likely tend to internalize other people’s emotions or let intrusive arrows (see the second blog in this 3-part series) right into your inner world. It often leads to feelings of resentment, frustration, shame, or sadness (etc.).
Flexible Boundaries: When we have flexible boundaries, we can easily adapt to different situations in our relationships with others. Our boundaries are clear, healthy, and reflect our needs, desires, emotions, and values. We also maintain some openness to the other’s reality, thoughts, feelings, and needs. This creates a space in our relationships where it’s safe to discuss our thoughts, feelings, emotions, and desires and listen to the other and make adjustments to fulfill both parties. It also creates respect within your relationship and brings you closer together. Lastly, flexible boundaries prevent you from feeling overwhelmed or building up resentment, all while letting other people in, creating a secure attachment, and fulfilling your needs.
We must establish a boundary to get to know who we are and what we need in our relationships to maintain a sense of safety and security and a sense of value and worth. Flexible boundaries might be ideal in relationships.
Mélodie Brown, B.A., is a therapist and completing a clinical psychology doctorate (D.Psy). At Centre for Interpersonal Relationships, she provides psychological services to adults and couples under the supervision of Dr. Dino Zuccarini, C.Psych. In the last year of her clinical psychology doctorate, Mélodie has completed all of her clinical training. She is in the process of finishing her thesis before receiving her licence as a clinical psychologist.